Diabetes is a chronic condition that affects millions worldwide, and when left unchecked, it can have devastating consequences on nearly every organ system in the body. Uncontrolled diabetes, whether type 1 or type 2, can lead to severe complications that develop gradually over months and years. Understanding how uncontrolled diabetes symptoms manifest and progress is essential for individuals living with the disease, as well as for healthcare professionals seeking to mitigate its impact. Research continually uncovers new insights into the mechanisms by which prolonged hyperglycemia causes damage, and these findings underscore the urgency of early detection and management.
You may also like: How Diabetes Affects the Brain: Understanding Brain Fog, Memory Loss, and Mental Confusion from High Blood Sugar
The Mechanisms of Uncontrolled Diabetes and Their Impact on the Body
At its core, diabetes is characterized by an inability of the body to properly regulate blood glucose levels. In uncontrolled diabetes, persistently high blood sugar can overwhelm the body’s regulatory mechanisms, leading to oxidative stress, inflammation, and vascular damage. The medical term for uncontrolled diabetes is hyperglycemia, a condition in which excess glucose in the bloodstream contributes to systemic dysfunction. Over time, these metabolic disturbances trigger a cascade of complications that affect multiple organs, leading to serious health consequences.
The body relies on insulin, a hormone produced by the pancreas, to facilitate the uptake of glucose into cells for energy. In type 1 diabetes, the immune system mistakenly attacks the insulin-producing beta cells in the pancreas, leading to an absolute deficiency of insulin. In type 2 diabetes, insulin resistance develops, making it difficult for cells to absorb glucose effectively. Regardless of the type, when blood sugar remains uncontrolled for prolonged periods, it sets off pathological changes that damage nerves, blood vessels, and vital organs.

Early Symptoms of Uncontrolled Diabetes: Recognizing the Warning Signs
One of the greatest dangers of uncontrolled diabetes is that it can progress silently, with symptoms appearing gradually. Among the earliest signs of uncontrolled diabetes are excessive thirst (polydipsia) and frequent urination (polyuria). These symptoms occur as the kidneys attempt to remove excess glucose from the bloodstream through urine. Increased hunger (polyphagia) is also common, as the body struggles to obtain sufficient energy despite high blood sugar levels.
Another hallmark symptom of uncontrolled diabetes is unexplained weight loss, particularly in type 1 diabetes. When glucose cannot be used for energy, the body resorts to breaking down fat and muscle for fuel. Additionally, individuals may experience chronic fatigue, blurred vision, and slow-healing wounds, which are all indicative of the body’s inability to manage high blood sugar levels effectively. Recognizing these early warning signs is crucial for preventing long-term complications.
The Cardiovascular Consequences of Uncontrolled Diabetes
One of the most significant and life-threatening complications of uncontrolled diabetes is cardiovascular disease. Research indicates that individuals with diabetes are two to four times more likely to develop heart disease compared to those without the condition. Prolonged hyperglycemia damages the endothelial lining of blood vessels, leading to atherosclerosis, a condition in which fatty deposits build up within arterial walls. This process significantly increases the risk of heart attacks, strokes, and peripheral artery disease.
Hypertension is another common consequence of uncontrolled diabetes, as elevated blood sugar levels contribute to stiffened and narrowed arteries. High blood pressure further exacerbates cardiovascular strain, creating a vicious cycle of worsening heart health. Studies suggest that aggressive blood sugar control and lifestyle modifications can reduce cardiovascular complications, highlighting the importance of maintaining glucose levels within target ranges.
Nerve Damage: Understanding Diabetic Neuropathy
Diabetic neuropathy is a debilitating condition that results from prolonged nerve damage due to high blood sugar. It is estimated that nearly half of individuals with diabetes will develop some form of neuropathy during their lifetime. The condition primarily affects the peripheral nerves, leading to symptoms such as tingling, burning sensations, numbness, and pain in the extremities.
Autonomic neuropathy, another form of nerve damage associated with uncontrolled diabetes, affects involuntary bodily functions such as digestion, heart rate, and blood pressure regulation. Individuals with autonomic neuropathy may experience issues such as gastroparesis (delayed stomach emptying), orthostatic hypotension (a drop in blood pressure when standing), and bladder dysfunction. Effective blood sugar control is key to slowing the progression of neuropathy and minimizing discomfort.
Kidney Disease: How Uncontrolled Diabetes Leads to Nephropathy
Diabetic nephropathy, or kidney disease, is another serious complication of uncontrolled diabetes. The kidneys contain tiny filtering units called nephrons that are responsible for removing waste from the blood. High blood sugar levels damage these nephrons over time, leading to decreased kidney function and, in severe cases, kidney failure.
Proteinuria, or the presence of excess protein in the urine, is often an early indicator of diabetic kidney disease. As nephropathy progresses, individuals may experience swelling in the legs and feet, fatigue, and difficulty concentrating due to toxin buildup in the bloodstream. Managing blood sugar and blood pressure is critical in preventing the progression of diabetic nephropathy, as uncontrolled diabetes remains a leading cause of end-stage renal disease requiring dialysis or kidney transplantation.
The Link Between Uncontrolled Diabetes and Vision Loss
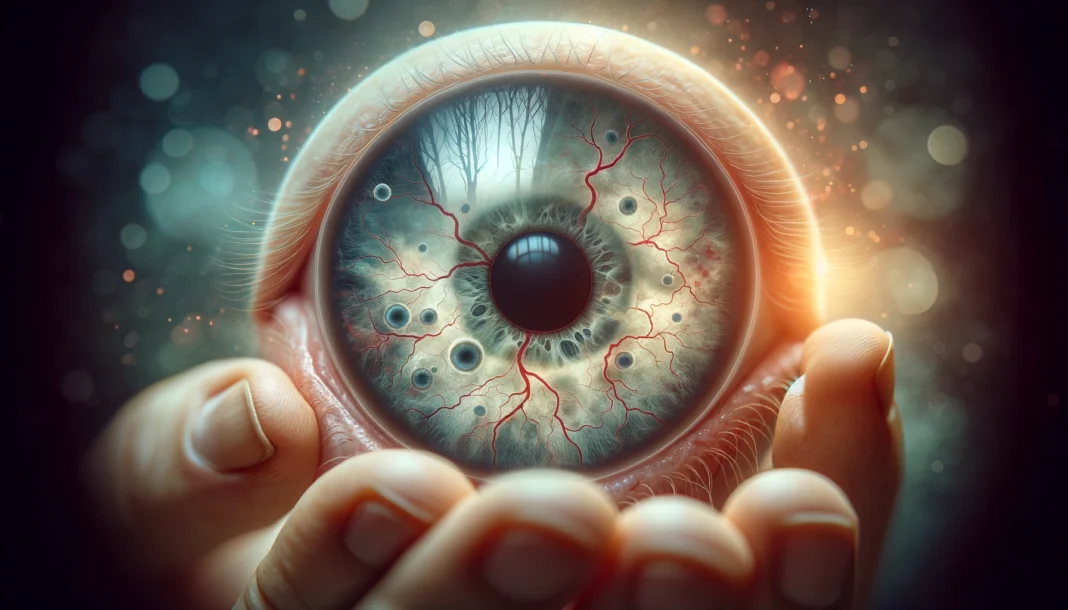
Another devastating consequence of prolonged hyperglycemia is diabetic retinopathy, a condition that affects the small blood vessels in the retina. Over time, high blood sugar levels weaken these vessels, causing them to leak fluid or bleed, leading to vision impairment. In its early stages, diabetic retinopathy may cause only mild symptoms, such as floaters or blurred vision, but if left untreated, it can progress to complete blindness.
Diabetes also increases the risk of other eye conditions, including cataracts and glaucoma. Cataracts develop more frequently in individuals with diabetes due to excess glucose forming deposits in the lens of the eye, leading to clouding and reduced vision. Glaucoma, characterized by increased intraocular pressure, can further damage the optic nerve, compounding vision loss. Regular eye exams are essential for detecting and managing these complications before they become severe.
The Impact of Uncontrolled Diabetes on the Immune System
Uncontrolled diabetes weakens the immune system, making individuals more susceptible to infections. High blood sugar impairs the function of white blood cells, which play a crucial role in fighting off bacteria and viruses. This diminished immune response increases the risk of skin infections, urinary tract infections, and more serious complications such as diabetic foot ulcers.
Diabetic foot ulcers, in particular, are a significant concern for individuals with long-term diabetes. Poor circulation, combined with nerve damage, results in wounds that heal slowly and are prone to infection. In severe cases, untreated infections can lead to gangrene and necessitate amputation. Maintaining strict blood sugar control and practicing good foot care can help prevent these complications.
Frequently Asked Questions: Uncontrolled Diabetes – Advanced Insights
1. Can uncontrolled diabetes influence cognitive function over time?
Yes, growing research links uncontrolled diabetes with both short-term and long-term cognitive decline. Chronic hyperglycemia can impair cerebral blood flow and damage small vessels in the brain, potentially leading to memory loss, difficulty concentrating, and even early onset dementia. These neurological effects often go unnoticed in early stages, making routine assessments crucial. Uncontrolled dm symptoms aren’t just physical—they can also manifest cognitively, impacting daily decision-making and emotional regulation. Understanding how diabetes affects the body beyond glucose metabolism is essential, especially for individuals at risk for Alzheimer’s disease, sometimes referred to as “type 3 diabetes” in academic circles due to these associations.
2. How does unmanaged stress impact uncontrolled diabetes symptoms?
Unmanaged psychological stress can significantly worsen uncontrolled diabetes symptoms by elevating cortisol levels, which increase blood glucose. Stress also disrupts sleep, appetite, and adherence to medication or dietary plans—all key pillars in diabetes management. In many cases, patients with uncontrolled dm report feeling overwhelmed or emotionally drained, which further contributes to poor self-care behaviors. Chronic stress compounds how diabetes affects the body, influencing both immune responses and cardiovascular health. Integrating mindfulness, cognitive behavioral therapy, or even structured exercise into daily routines can reduce these stress-driven glycemic spikes and improve overall metabolic stability.
3. What is the long-term cardiovascular risk associated with uncontrolled dm?
The long-term cardiovascular consequences of uncontrolled dm are among the most serious complications of the condition. Chronic high blood sugar accelerates atherosclerosis, increases arterial stiffness, and promotes endothelial dysfunction. As a result, individuals with uncontrolled diabetes face significantly higher risks for heart attacks, strokes, and peripheral artery disease. These aren’t just distant threats—subclinical heart damage can begin within a few years of poor glycemic control. Recognizing subtle uncontrolled dm symptoms, such as unexplained fatigue or swelling in the lower extremities, can be key to early cardiovascular intervention.
4. How do sleep disorders interact with uncontrolled diabetes?
Sleep disturbances like insomnia, restless leg syndrome, and obstructive sleep apnea are increasingly recognized as both causes and consequences of uncontrolled diabetes. Poor sleep quality disrupts glucose metabolism and heightens insulin resistance, worsening uncontrolled diabetes symptoms. Conversely, high blood sugar levels can cause nocturia, night sweats, and neuropathic pain that interrupt sleep. This bidirectional relationship exemplifies how diabetes affects the body in ways that are often overlooked. Addressing sleep hygiene, undergoing sleep studies, or adjusting medications may help break this cycle and support better glycemic control.
5. Can uncontrolled diabetes alter gut microbiota composition?
Emerging research suggests that uncontrolled diabetes can significantly shift the composition of gut microbiota. These microbial imbalances may worsen inflammation, insulin resistance, and gastrointestinal symptoms like bloating or diarrhea. This gut dysbiosis is now being explored as both a consequence and a potential contributor to how diabetes affects the body. Studies show that patients with uncontrolled dm often have lower levels of beneficial bacteria like Akkermansia muciniphila and Faecalibacterium prausnitzii. Probiotic therapy, dietary fiber, and resistant starch intake may offer novel adjunct strategies for improving metabolic outcomes alongside traditional treatment.
6. Is there a connection between uncontrolled diabetes and vision loss beyond retinopathy?
While diabetic retinopathy is well-known, uncontrolled diabetes can also affect vision through mechanisms like lens swelling (leading to fluctuating vision), glaucoma, and cataracts. Uncontrolled dm symptoms such as persistent blurred vision or halos around lights may indicate these secondary eye complications. Moreover, rapid changes in blood sugar levels can distort fluid balance in the eye, temporarily impairing focus. Patients with prolonged uncontrolled diabetes should undergo comprehensive eye exams at least annually—not only retinal screenings—to assess intraocular pressure, corneal health, and lens clarity.
7. How does social isolation impact individuals living with uncontrolled diabetes?
Social isolation, particularly among older adults or those with mobility limitations, can worsen both the mental and physical outcomes of uncontrolled diabetes. Isolation reduces access to support systems critical for medication adherence, meal planning, and emergency response. Additionally, loneliness has been shown to elevate inflammatory markers and stress hormones that exacerbate uncontrolled diabetes symptoms. The psychological toll of isolation may increase the risk of depression, further reducing engagement in self-care behaviors. Integrating community-based programs or digital health support can bridge this gap and improve quality of life.
8. Are there gender-specific differences in how uncontrolled diabetes presents?
Yes, uncontrolled diabetes symptoms can differ between men and women. Women may experience more frequent urinary tract infections, yeast infections, and fluctuations in hormone-related blood sugar levels. Men, on the other hand, may be more likely to overlook early symptoms or present with erectile dysfunction as a vascular complication. The way uncontrolled dm manifests can also be influenced by hormonal shifts during menopause or andropause, complicating diagnosis and management. Personalized treatment strategies that account for sex-specific physiological and psychosocial factors are essential for optimal care.
9. What innovations are emerging for the treatment of uncontrolled diabetes?
Innovations in diabetes care are rapidly evolving to address the challenges of uncontrolled diabetes. Continuous glucose monitoring (CGM), closed-loop insulin delivery systems, and AI-driven decision-support tools are redefining how we manage blood sugar. Novel therapies targeting GLP-1 receptors, GIP co-agonists, and SGLT2 inhibitors show promise in improving metabolic control with fewer side effects. These advancements are not just technological—they reflect a deeper understanding of how diabetes affects the body at the molecular and systemic levels. For those with uncontrolled dm symptoms despite standard care, these breakthroughs could represent a critical turning point.
10. Why is it important to distinguish between uncontrolled diabetes and poorly managed diabetes?
While often used interchangeably, “uncontrolled diabetes” and “poorly managed diabetes” can imply different clinical realities. Uncontrolled diabetes may result from factors beyond patient control, such as autoimmune disease progression, medication resistance, or coexisting illnesses. In contrast, poorly managed diabetes often refers to behavioral or systemic issues like non-adherence, lack of access to care, or educational gaps. Understanding this distinction is important because the medical term for uncontrolled diabetes encompasses both physiologic and social determinants of health. Effective treatment requires personalized strategies that address both the medical term for uncontrolled diabetes and its real-world implications for the patient.
Conclusion: The Importance of Early Intervention and Continuous Management
The impact of uncontrolled diabetes on the body is far-reaching and potentially life-threatening. From cardiovascular disease and neuropathy to kidney failure and vision loss, the consequences of prolonged hyperglycemia can significantly reduce quality of life. However, early detection and proactive management can help prevent or slow the progression of these complications. Scientific research underscores the importance of maintaining optimal blood sugar levels through a combination of medication, dietary modifications, and lifestyle changes.
For individuals living with diabetes, regular monitoring and adherence to treatment plans are crucial. Ongoing medical advancements continue to improve diabetes management, offering hope for better outcomes and a higher quality of life. Education, awareness, and access to proper healthcare resources are essential in empowering individuals to take control of their condition and minimize the risks associated with uncontrolled diabetes.
diabetes complications, diabetic neuropathy symptoms, chronic hyperglycemia effects, diabetic retinopathy causes, cardiovascular disease and diabetes, kidney damage from diabetes, insulin resistance complications, diabetic foot ulcers treatment, blood sugar control strategies, hypertension and diabetes, metabolic syndrome risks, type 2 diabetes progression, diabetic nephropathy prevention, oxidative stress and diabetes, vision loss due to diabetes, immune system and diabetes, long-term effects of diabetes, diabetes-related nerve pain, early signs of uncontrolled diabetes, diabetes management strategies
Further Reading:
Effects of diabetes on the body and organs
Type 2 Diabetes and its Impact on the Immune System
10 signs of uncontrolled diabetes
Disclaimer: The content published on Better Nutrition News (https://betternutritionnews.com) is for informational and educational purposes only. It is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the guidance of a qualified healthcare professional before making any changes to your diet, nutrition, or wellness practices. The opinions expressed by authors and contributors are their own and do not necessarily reflect those of Better Nutrition News.
Better Nutrition News and its affiliates make no representations or warranties regarding the accuracy, completeness, or reliability of the information provided. We disclaim all liability for any loss, injury, or damage resulting from the use or reliance on the content published on this site. External links are provided for reference purposes only and do not imply endorsement.